26 results
Vitamin K1 intake and incident diabetes in the Danish Diet Cancer and Health study
- P. Pokharel, J.W. Bellinge, F. Dalgaard, K. Murray, M. Sim, B. Yeap, E. Connolly, L. Blekkenhorst, C. Bondonno, J. Lewis, G. Gislason, A. Tjønneland, K. Overvad, J. Hodgson, C. Schultz, N. Bondonno
-
- Journal:
- Proceedings of the Nutrition Society / Volume 82 / Issue OCE2 / 2023
- Published online by Cambridge University Press:
- 22 March 2023, E177
-
- Article
-
- You have access Access
- HTML
- Export citation
In situ, broadband measurement of the radio frequency attenuation length at Summit Station, Greenland
- J. A. Aguilar, P. Allison, J. J. Beatty, D. Besson, A. Bishop, O. Botner, S. Bouma, S. Buitink, M. Cataldo, B. A. Clark, Z. Curtis-Ginsberg, A. Connolly, P. Dasgupta, S. de Kockere, K. D. de Vries, C. Deaconu, M. A. DuVernois, C. Glaser, A. Hallgren, S. Hallmann, J. C. Hanson, B. Hendricks, C. Hornhuber, K. Hughes, A. Karle, J. L. Kelley, I. Kravchenko, R. Krebs, R. Lahmann, U. Latif, J. Mammo, Z. S. Meyers, K. Michaels, K. Mulrey, A. Nelles, A. Novikov, A. Nozdrina, E. Oberla, B. Oeyen, Y. Pan, H. Pandya, I. Plaisier, N. Punsuebsay, L. Pyras, D. Ryckbosch, O. Scholten, D. Seckel, M. F. H. Seikh, D. Smith, D. Southall, J. Torres, S. Toscano, D. Tosi, D. J. Van Den Broeck, N. van Eijndhoven, A. G. Vieregg, C. Welling, D. R. Williams, S. Wissel, R. Young, A. Zink
-
- Journal:
- Journal of Glaciology / Volume 68 / Issue 272 / December 2022
- Published online by Cambridge University Press:
- 30 May 2022, pp. 1234-1242
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Over the last 25 years, radiowave detection of neutrino-generated signals, using cold polar ice as the neutrino target, has emerged as perhaps the most promising technique for detection of extragalactic ultra-high energy neutrinos (corresponding to neutrino energies in excess of 0.01 Joules, or 1017 electron volts). During the summer of 2021 and in tandem with the initial deployment of the Radio Neutrino Observatory in Greenland (RNO-G), we conducted radioglaciological measurements at Summit Station, Greenland to refine our understanding of the ice target. We report the result of one such measurement, the radio-frequency electric field attenuation length $L_\alpha$
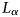 . We find an approximately linear dependence of $L_\alpha$
. We find an approximately linear dependence of $L_\alpha$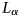 on frequency with the best fit of the average field attenuation for the upper 1500 m of ice: $\langle L_\alpha \rangle = ( ( 1154 \pm 121) - ( 0.81 \pm 0.14) \, ( \nu /{\rm MHz}) ) \,{\rm m}$
on frequency with the best fit of the average field attenuation for the upper 1500 m of ice: $\langle L_\alpha \rangle = ( ( 1154 \pm 121) - ( 0.81 \pm 0.14) \, ( \nu /{\rm MHz}) ) \,{\rm m}$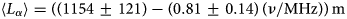 for frequencies ν ∈ [145 − 350] MHz.
for frequencies ν ∈ [145 − 350] MHz.
P.120 Case series: Clinical and genetic spectrum of SCN8A-related disorders in British Columbia
- M Hebbar, N Al-Taweel, I Gill, C Boelman, RA Dean, SJ Goodchild, J Mezeyova, NG Shuart, JP Johnson, Jr., J Lee, A Michoulas, LL Huh, L Armstrong, MB Connolly, M Demos
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 48 / Issue s3 / November 2021
- Published online by Cambridge University Press:
- 05 January 2022, p. S53
-
- Article
-
- You have access Access
- Export citation
-
Background: Children with pathogenic variations in SCN8A can present with early infantile epileptic encephalopathy-13, benign familial infantile seizures-5 or intellectual disability alone without epilepsy. In this case series, we discuss six children with variants in SCN8A managed at BC Children’s Hospital. Methods: We describe clinical and genetic results on six individuals with SCN8A variants identified via clinical or research next-generation sequencing. Functional consequences of two SCN8A variants were assessed using electrophysiological analyses in transfected cells. Results: Clinical findings ranged from normal development with well-controlled epilepsy to significant developmental delay with treatment-resistant epilepsy. Phenotypes and genotypes in our cohort are described in the table below. Functional analysis supported gain-of-function in P2 and loss-of-function in P4. Conclusions: Our cohort expands the clinical and genotypic spectrum of SCN8A-related disorders. We establish functional evidence for two missense variants in SCN8A, including LoF variant in a patient with intellectual disability, and autism spectrum disorder without seizures.
Table for P.120
Patients Age/Sex Development Age of seizure onset Epilepsy type Current antiseizure medication Seizure frequency Gene variant/Function Inheritance P1 14y/F Profound GDD 5m Infantile spasms, LGS, hyperkinetic movements Clobazam Daily c.1238C>A (p.Ala413Asp) De novo P2 6y/F Normal 3-7m Focal epilepsy Carbamazepine Seizure free c.5630A>G (p.Asn1877Ser)/GoF Paternal P3 4y/F Normal 12m Focal epilepsy Clobazam, topiramate Seizure free c.4447G>A (p.Glu1483Lys) De novo P4 6y/F GDD, autism 3y - EEG abnormality only - Sodium valproate (discontinued) No clinical seizure c.971G>A (p.Cys324Tyr)/LoF, VUS in KCNQ3 De novo P5 7y/M GDD 5m Generalized seizures Ethosuximide, acetazolamide Daily c.773C>T (p.Thr258Ile) De novo P6 19y/F Normal 10y Focal epilepsy Carba mazepine Seizure free c.986A>G (p.Asp329Gly) De novo Abbreviations: *Father with similar history, y Years, m Months, GDD Global developmental delay, LGS Lennox-Gastaut syndrome, VUS Variant of unknown significance, LoF Loss-of-function, GoF Gain-of-function, EEG Electroencephalogram, F - Female, M - Male, CBD - Cannabidiol
Interactive impact of childhood maltreatment, depression, and age on cortical brain structure: mega-analytic findings from a large multi-site cohort
- Leonardo Tozzi, Lisa Garczarek, Deborah Janowitz, Dan J. Stein, Katharina Wittfeld, Henrik Dobrowolny, Jim Lagopoulos, Sean N. Hatton, Ian B. Hickie, Angela Carballedo, Samantha J. Brooks, Daniella Vuletic, Anne Uhlmann, Ilya M. Veer, Henrik Walter, Robin Bülow, Henry Völzke, Johanna Klinger-König, Knut Schnell, Dieter Schoepf, Dominik Grotegerd, Nils Opel, Udo Dannlowski, Harald Kugel, Elisabeth Schramm, Carsten Konrad, Tilo Kircher, Dilara Jüksel, Igor Nenadić, Axel Krug, Tim Hahn, Olaf Steinsträter, Ronny Redlich, Dario Zaremba, Bartosz Zurowski, Cynthia H.Y. Fu, Danai Dima, James Cole, Hans J. Grabe, Colm G. Connolly, Tony T. Yang, Tiffany C. Ho, Kaja Z. LeWinn, Meng Li, Nynke A. Groenewold, Lauren E. Salminen, Martin Walter, Alan N Simmons, Theo G.M. van Erp, Neda Jahanshad, Bernhard T. Baune, Nic J.A. van der Wee, Marie-Jose van Tol, Brenda W.J.H. Penninx, Derrek P. Hibar, Paul M. Thompson, Dick J. Veltman, Lianne Schmaal, Thomas Frodl, ‘for the ENIGMA-MDD Consortium’
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 6 / April 2020
- Published online by Cambridge University Press:
- 14 May 2019, pp. 1020-1031
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Childhood maltreatment (CM) plays an important role in the development of major depressive disorder (MDD). The aim of this study was to examine whether CM severity and type are associated with MDD-related brain alterations, and how they interact with sex and age.
MethodsWithin the ENIGMA-MDD network, severity and subtypes of CM using the Childhood Trauma Questionnaire were assessed and structural magnetic resonance imaging data from patients with MDD and healthy controls were analyzed in a mega-analysis comprising a total of 3872 participants aged between 13 and 89 years. Cortical thickness and surface area were extracted at each site using FreeSurfer.
ResultsCM severity was associated with reduced cortical thickness in the banks of the superior temporal sulcus and supramarginal gyrus as well as with reduced surface area of the middle temporal lobe. Participants reporting both childhood neglect and abuse had a lower cortical thickness in the inferior parietal lobe, middle temporal lobe, and precuneus compared to participants not exposed to CM. In males only, regardless of diagnosis, CM severity was associated with higher cortical thickness of the rostral anterior cingulate cortex. Finally, a significant interaction between CM and age in predicting thickness was seen across several prefrontal, temporal, and temporo-parietal regions.
ConclusionsSeverity and type of CM may impact cortical thickness and surface area. Importantly, CM may influence age-dependent brain maturation, particularly in regions related to the default mode network, perception, and theory of mind.
COST ANALYSIS OF PERIPHERALLY INSERTED CENTRAL CATHETER IN PEDIATRIC PATIENTS
- Zhaoxin Dong, Bairbre L. Connolly, Wendy J. Ungar, Peter C. Coyte
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 34 / Issue 1 / 2018
- Published online by Cambridge University Press:
- 20 December 2017, pp. 38-45
-
- Article
- Export citation
-
Purpose: A peripherally inserted central catheter (PICC) is a useful option in providing secure venous access, which enables patients to be discharged earlier with the provision of home care. The objective was to identify the costs associated with having a PICC from a societal perspective, and to identify factors that are associated with total PICC costs.
Methods: Data were obtained from a retrospective cohort of 469 hospitalized pediatric patients with PICCs inserted. Both direct and indirect costs were estimated from a societal perspective. Insertion costs, complication costs, nurse and physician assessment costs, inpatient ward costs, catheter removal costs, home care costs, travel costs, and the cost associated with productivity losses incurred by parents were included in this study.
Results: Based on catheter dwell time, the median total cost associated with a PICC per patient per day (including inpatient hospital costs) was $3,133.5 ($2,210.7–$9,627.0) in 2017 Canadian dollars ($1.00USD = $1.25CAD in 2017). The adjusted mean cost per patient per day was $2,648.2 ($2,402.4–$2,920.4). Excluding inpatient ward costs, the median total and adjusted costs per patient per day were $198.8 ($91.8–$2,475.8) and $362.7($341.0–$386.0), respectively. Younger age, occurrence of complications, more catheter dwell days, wards with more intensive care, and the absence of home care were significant factors associated with higher total PICC costs.
Conclusions: This study has demonstrated the costs associated with PICCs. This information may be helpful for healthcare providers to understand PICC related cost in children and resource implications.
LO36: Out-of-hospital cardiac arrest in British Columbia: Ten years of increasing survival
- B.E. Grunau, W. Dick, T. Kawano, F.X. Scheuermeyer, C. Fordyce, D. Barbic, R. Straight, R. Schlamp, H. Connolly, J. Christenson
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S40
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Survival for victims of out-of-hospital cardiac arrest (OHCA) is typically between 8 and 12%. We sought to report the trends in survival in British Columbia (BC) over a 10-year period. Methods: The BC Resuscitation Outcomes Consortium prospectively collected detailed prehospital and hospital data on consecutive non-traumatic OHCAs from 2006 to 2016 within BC’s four metropolitan areas. We included EMS-treated adult patients without DNR orders. To describe baseline characteristics we organized patient characteristics in three time periods: 2006-09, 2010-13, and 2014-16 (first and last periods reported below). The primary and secondary endpoints were survival at hospital discharge and return of spontaneous circulation (ROSC). We tested the significance of year-by-year trends in baseline characteristics, and performed multivariable Poisson regression, using calendar year as an independent variable, to calculate risk-adjusted rates for survival. Results: Between January 1, 2006 and March 31, 2016 there were a total of 26 433 non-traumatic OHCAs, with 15 145 included in this study. There were significant decreases in the proportion with initial shockable cardiac rhythms (28% to 23%) and bystander witnessed arrests (42% to 39%), however significant increases in the proportion with bystander CPR (40% to 49%) and ALS treatment (86% to 97%), and the median chest compression fraction (0.81 to 0.87). There was a significant increase in the median time until termination of resuscitation in those who did not achieve ROSC (27 to 32 minutes), and a significant decrease in the proportion of patients who were transported in absence of ROSC (17% to 6.5%). There was a significant improvement in achieving ROSC (44% to 48%; adjusted rate ratio per year 1.02, 95% CI 1.01 to 1.02) and survival at hospital discharge (10% to 14%; adjusted rate ratio per year 1.05, 95% CI 1.04 to 1.06). Both subgroups of initial shockable (adjusted rate ratio per year 1.04, 95% CI 1.03 to 1.05) and non-shockable (adjusted rate ratio per year 1.08, 95% CI 1.06 to 1.12) cardiac rhythms demonstrated survival improvement. Conclusion: Despite a significant decrease in those with initial shockable rhythms, out-of-hospital cardiac arrest survival in BC’s metropolitan regions increased by approximately 40% over a 10-year period. During this time there were system changes and quality of care improvements as provided by bystanders and professionals.
LO44: Initial validation of the core components in the SHoC-Hypotension Protocol. What rates of ultrasound findings are reported in emergency department patients with undifferentiated hypotension? Results from the first Sonography in Hypotension and Cardiac Arrest in the Emergency Department (SHOC-ED1) Study; an international randomized controlled trial
- D. Lussier, C. Pham, J. Milne, D. Lewis, L. Diegelmann, H. Lamprecht, R. Henneberry, J. Fraser, M. Stander, D.J. van Hoving, D. Fredericks, M. Howlett, J. Mekwan, B. Ramrattan, J. Middleton, P. Olszynski, M. Peach, L. Taylor, T. Dahn, S.T. Hurley, K. MacSween, C. Cox, S. Hunter, J. Bowra, M. Lambert, R. Jarman, T. Harris, V. Noble, J. Connolly, P.R. Atkinson
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, pp. S42-S43
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Point of care ultrasound (PoCUS) has become an established tool in the initial management of patients with undifferentiated hypotension in the emergency department (ED). Current established protocols (e.g. RUSH and ACES) were developed by expert user opinion, rather than objective, prospective data. Recently the SHoC Protocol was published, recommending 3 core scans; cardiac, lung, and IVC; plus other scans when indicated clinically. We report the abnormal ultrasound findings from our international multicenter randomized controlled trial, to assess if the recommended 3 core SHoC protocol scans were chosen appropriately for this population. Methods: Recruitment occurred at seven centres in North America (4) and South Africa (3). Screening at triage identified patients (SBP<100 or shock index>1) who were randomized to PoCUS or control (standard care with no PoCUS) groups. All scans were performed by PoCUS-trained physicians within one hour of arrival in the ED. Demographics, clinical details and study findings were collected prospectively. A threshold incidence for positive findings of 10% was established as significant for the purposes of assessing the appropriateness of the core recommendations. Results: 138 patients had a PoCUS screen completed. All patients had cardiac, lung, IVC, aorta, abdominal, and pelvic scans. Reported abnormal findings included hyperdynamic LV function (59; 43%); small collapsing IVC (46; 33%); pericardial effusion (24; 17%); pleural fluid (19; 14%); hypodynamic LV function (15; 11%); large poorly collapsing IVC (13; 9%); peritoneal fluid (13; 9%); and aortic aneurysm (5; 4%). Conclusion: The 3 core SHoC Protocol recommendations included appropriate scans to detect all pathologies recorded at a rate of greater than 10 percent. The 3 most frequent findings were cardiac and IVC abnormalities, followed by lung. It is noted that peritoneal fluid was seen at a rate of 9%. Aortic aneurysms were rare. This data from the first RCT to compare PoCUS to standard care for undifferentiated hypotensive ED patients, supports the use of the prioritized SHoC protocol, though a larger study is required to confirm these findings.
LO042: Sonography in Hypotension and Cardiac Arrest (SHoC) - Hypotension: derivation of an evidence-based consensus algorithm for the integration of point of care ultrasound into resuscitation of hypotensive patients
- P. Atkinson, J. Bowra, J. Milne, M. Lambert, B. Jarman, V. Noble, H. Lamprecht, D. Lewis, T. Harris, R. Gangahar, Advisory panel members , M. Stander, C. Muhr, J. Connolly, R. Gaspari, R. Kessler, C. Raio, P. Sierzenski, B. Hoffmann, C. Pham, M. Woo, P. Olszynski, R. Henneberry, O. Frenkel, J. Chenkin, G. Hall, L. Rang, M. Valois, C. Wurster, M. Tutschka, R. Arntfield, J. Fischer, M. Tessaro
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 18 / Issue S1 / May 2016
- Published online by Cambridge University Press:
- 02 June 2016, p. S44
- Print publication:
- May 2016
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Point of care ultrasound has become an established tool in the initial management of patients with undifferentiated hypotension. Current established protocols (RUSH, ACES, etc) were developed by expert user opinion, rather than objective, prospective data. We wished to use reported disease incidence to develop an informed approach to PoCUS in hypotension using a “4 F’s” approach: Fluid; Form; Function; Filling. Methods: We summarized the incidence of PoCUS findings from an international multicentre RCT, and using a modified Delphi approach incorporating this data we obtained the input of 24 international experts associated with five professional organizations led by the International Federation of Emergency Medicine. The modified Delphi tool was developed to reach an international consensus on how to integrate PoCUS for hypotensive emergency department patients. Results: Rates of abnormal PoCUS findings from 151 patients with undifferentiated hypotension included left ventricular dynamic changes (43%), IVC abnormalities (27%), pericardial effusion (16%), and pleural fluid (8%). Abdominal pathology was rare (fluid 5%, AAA 2%). After two rounds of the survey, using majority consensus, agreement was reached on a SHoC-hypotension protocol comprising: A. Core: 1. Cardiac views (Sub-xiphoid and parasternal windows for pericardial fluid, cardiac form and ventricular function); 2. Lung views for pleural fluid and B-lines for filling status; and 3. IVC views for filling status; B. Supplementary: Additional cardiac views; and C. Additional views (when indicated) including peritoneal fluid, aorta, pelvic for IUP, and proximal leg veins for DVT. Conclusion: An international consensus process based on prospectively collected disease incidence has led to a proposed SHoC-hypotension PoCUS protocol comprising a stepwise clinical-indication based approach of Core, Supplementary and Additional PoCUS views.
LO045: Sonography in Hypotension and Cardiac Arrest (SHoC) - Cardiac Arrest: A consensus on the integration of point of care ultrasound into advanced cardiac life support during cardiac arrest
- P. Atkinson, J. Bowra, J. Milne, M. Lambert, B. Jarman, V. Noble, H. Lamprecht, D. Lewis, T. Harris, R. Gangahar, Advisory panel members , S. Bomann, A. Goudie, H. Poncia, A. Bystrzycki, G. Blecher, M. Rose, S. Dass, O. Doran, R. Large, A. Salter, J. Sadewasser, A. Murray, M. Rawson, M. Stander, C. Muhr, J. Connolly, R. Gaspari, R. Kessler, C. Raio, P. Sierzenski, B. Hoffmann, C. Pham, M. Woo, P. Olszynski, R. Henneberry, O. Frenkel, J. Chenkin, G. Hall, L. Rang, M. Valois, C. Wurster, M. Tutschka, R. Arntfield, J. Fischer, M. Tessaro
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 18 / Issue S1 / May 2016
- Published online by Cambridge University Press:
- 02 June 2016, pp. S45-S46
- Print publication:
- May 2016
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Point of care ultrasound (PoCUS) provides invaluable information during resuscitation efforts in cardiac arrest by determining presence/absence of cardiac activity and identifying reversible causes such as pericardial tamponade. There is no agreed guideline on how to safely and effectively incorporate PoCUS into the advanced cardiac life support (ACLS) algorithm. We consider that a consensus-based priority checklist using a “4 F’s” approach (Fluid; Form; Function; Filling), would provide a better algorithm during ACLS. Methods: The ultrasound subcommittee of the Australasian College for Emergency Medicine (ACEM) drafted a checklist incorporating PoCUS into the ACLS algorithm. This was further developed using the input of 24 international experts associated with five professional organizations led by the International Federation of Emergency Medicine. A modified Delphi tool was developed to reach an international consensus on how to integrate ultrasound into cardiac arrest algorithms for emergency department patients. Results: Consensus was reached following 3 rounds. The agreed protocol focuses on the timing of PoCUS as well as the specific clinical questions. Core cardiac windows performed during the rhythm check pause in chest compressions are the sub-xiphoid and parasternal cardiac views. Either view should be used to detect pericardial fluid, as well as examining ventricular form (e.g. right heart strain) and function, (e.g. asystole versus organized cardiac activity). Supplementary views include lung views (for absent lung sliding in pneumothorax and for pleural fluid), and IVC views for filling. Additional ultrasound applications are for endotracheal tube confirmation, proximal leg veins for DVT, or for sources of blood loss (AAA, peritoneal/pelvic fluid). Conclusion: The authors hope that this process will lead to a consensus-based SHoC-cardiac arrest guideline on incorporating PoCUS into the ACLS algorithm.
Infection Control Implications of Protracted Lengths of Stay With Noninfluenza Viral Influenza-Like Illnesses in Hospitalized Adults During the 2015 Influenza A (H3N2) Epidemic
- Burke A. Cunha, James J. Connolly, Adina C. Musta, Eileen Abruzzo
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 36 / Issue 11 / November 2015
- Published online by Cambridge University Press:
- 01 September 2015, pp. 1368-1370
- Print publication:
- November 2015
-
- Article
-
- You have access Access
- HTML
- Export citation
Utilization of transition care management plans to facilitate transition of adolescents with epilepsy into the adult healthcare system
- C Hrazdil, A Datta, A Michoulas, S Morgan, S Peinhof, K Selby, L Straatman, S Rabinovitz, A Chapman, D Evans, J Lachar, M Paone, A Sayao, S Whitehouse, W Woodfield, M Connolly
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 42 / Issue S1 / May 2015
- Published online by Cambridge University Press:
- 03 June 2015, p. S23
-
- Article
-
- You have access Access
- Export citation
-
Background: For adolescents with epilepsy, there is often a poor system in place to meet their individualized transition needs. Our objectives were 1) to develop epilepsy-specific transition care management plans (TCMPs) to ensure access, and attachment to adult healthcare providers, and 2) to identify strategies for providing support during the transition period, including through the development of physician and patient (or caregiver) navigated web-based tools, resources and recommendations for health system improvements. Methods: Physicians and nurses with expertise in areas including adult and pediatric epilepsy, family medicine, psychiatry, and varied allied health professionals were engaged to generate epilepsy-related TCMPs. Results: Through an iterative process spanning the course of over a year, TCMPs were developed to cover areas including: treatment responsive and resistant epilepsy, ketogenic diet, epilepsy surgery, women’s issues, mental health, and psychosocial aspects of epilepsy. The TCMPs referenced established guidelines and best practices in the literature wherever possible. Caregiver roles and responsibilities were outlined, remaining cognoscent of available provincial resources. Conclusions: Epilepsy specific TCMPs can be developed through a collaborative approach between pediatric and adult healthcare providers, easing the patient experience, creating educated accountability, and providing a forum to identify and address gaps of care in adolescents with epilepsy.
HIV Infection Is Associated with Attenuated Frontostriatal Intrinsic Connectivity: A Preliminary Study
- Jonathan C. Ipser, Gregory G. Brown, Amanda Bischoff-Grethe, Colm G. Connolly, Ronald J. Ellis, Robert K. Heaton, Igor Grant, Translational Methamphetamine AIDS Research Center (TMARC) Group
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 21 / Issue 3 / March 2015
- Published online by Cambridge University Press:
- 31 March 2015, pp. 203-213
-
- Article
- Export citation
-
HIV-associated cognitive impairments are prevalent, and are consistent with injury to both frontal cortical and subcortical regions of the brain. The current study aimed to assess the association of HIV infection with functional connections within the frontostriatal network, circuitry hypothesized to be highly vulnerable to HIV infection. Fifteen HIV-positive and 15 demographically matched control participants underwent 6 min of resting-state functional magnetic resonance imaging (RS-fMRI). Multivariate group comparisons of age-adjusted estimates of connectivity within the frontostriatal network were derived from BOLD data for dorsolateral prefrontal cortex (DLPFC), dorsal caudate and mediodorsal thalamic regions of interest. Whole-brain comparisons of group differences in frontostriatal connectivity were conducted, as were pairwise tests of connectivity associations with measures of global cognitive functioning and clinical and immunological characteristics (nadir and current CD4 count, duration of HIV infection, plasma HIV RNA). HIV – associated reductions in connectivity were observed between the DLPFC and the dorsal caudate, particularly in younger participants (<50 years, N=9). Seropositive participants also demonstrated reductions in dorsal caudate connectivity to frontal and parietal brain regions previously demonstrated to be functionally connected to the DLPFC. Cognitive impairment, but none of the assessed clinical/immunological variables, was also associated with reduced frontostriatal connectivity. In conclusion, our data indicate that HIV is associated with attenuated intrinsic frontostriatal connectivity. Intrinsic connectivity of this network may therefore serve as a marker of the deleterious effects of HIV infection on the brain, possibly via HIV-associated dopaminergic abnormalities. These findings warrant independent replication in larger studies. (JINS, 2015, 21, 1–11)
The Role of Polyamine Metabolism in Neuronal Injury Following Cerebral Ischemia
- Grace H. Kim, Ricardo J. Komotar, Margy E. McCullough-Hicks, Marc L. Otten, Robert M. Starke, Christopher P. Kellner, Matthew C. Garrett, Maxwell B. Merkow, Michal Rynkowski, Kelly A. Dash, E. Sander Connolly
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 36 / Issue 1 / January 2009
- Published online by Cambridge University Press:
- 02 December 2014, pp. 14-19
-
- Article
-
- You have access Access
- Export citation
-
Stroke is a leading cause of morbidity and mortality in the US, with secondary damage following the initial insult contributing significantly to overall poor outcome. Prior investigations have shown that the metabolism of certain polyamines such as spermine, spermidine, and putrescine are elevated in ischemic parenchyma, resulting in an increase in their metabolite concentration. Polyamine metabolites tend to be cytotoxic, leading to neuronal injury in the penumbra following stroke and expansion of the area of infarcted tissue. Although the precise mechanism is unclear, the presence of reactive aldehydes produced through polyamine metabolism, such as 3-aminopropanal and acrolein, have been shown to correlate with the incidence of cerebral vasospasm, disruption of oxidative metabolism and mitochondrial functioning, and disturbance of cellular calcium ion channels. Regulation of the polyamine metabolic pathway, therefore, may have the potential to limit injury following cerebral ischemia. To this end, we review this pathway in detail with an emphasis on clinical applicability.
Contributors
-
- By Federica Agosta, Alberto Albanese, Timothy J. Amrhein, A. M. Barrett, Walter S. Bartynski, Felix Benninger, Thomas Brandt, Andrew G. Burke, Michelle Cameron, Elisa Canu, Louis R. Caplan, Christine M. Carr, Daniel J. A. Connolly, Firouz Daneshgari, John DeLuca, Marianne de Visser, Marianne Dieterich, Antonio E. Elia, Joseph H. Feinberg, Massimo Filippi, Lauren C. Frey, Gaëtan Garraux, Andrea Ginestroni, Peter J. Goadsby, Bronwyn E. Hamilton, Simon J. Hickman, Holly E. Hinson, Jon P. Jennings, Jan Kassubek, Horacio Kaufmann, David M. Kaylie, Joanna Kitley, Vladimir S. Kostic, C. T. Paul Krediet, Megan C. Leary, Farooq H. Maniyar, Ken R. Maravilla, Mario Mascalchi, Rajarshi Mazumder, Priyesh Mehta, Jacqueline A. Palace, Raj M. Paspulati, Christopher A. Potter, Angelo Quattrini, Louis P. Riccelli, Nilo Riva, Maria A. Rocca, Mirabelle B. Sajisevi, Richard Salazar-Montero, Nicholas D. Schiff, Jack H. Simon, Israel Steiner, Carl D. Stevens, Bart P. van de Warrenburg, Judith van Gaalen, William J. Weiner, Jane L. Weissman, Jay Yao, G. Bryan Young
- Edited by Massimo Filippi, Jack H. Simon
-
- Book:
- Imaging Acute Neurologic Disease
- Published online:
- 05 October 2014
- Print publication:
- 11 September 2014, pp vi-viii
-
- Chapter
- Export citation
Cellular in vitro bioactivity of protein hydrolysates from brewers' spent grain
- A. L. McCarthy, Y. C. Ocallaghan, A. Connolly, C. O. Piggott, R. J. Fitzgerald, N. M. Obrien
-
- Journal:
- Proceedings of the Nutrition Society / Volume 72 / Issue OCE4 / 2013
- Published online by Cambridge University Press:
- 30 August 2013, E223
-
- Article
-
- You have access Access
- HTML
- Export citation
List of contributors
-
- By Mike Abbott, Jean-Jacques Amy, Deborah J. Bateson, Johannes Bitzer, Paula Briggs, Anne Connolly, David Crook, Tony Feltbower, Kathy French, Lynne Garforth, Ailsa E. Gebbie, Kristina Gemzell-Danielsson, Marie-Odile Gerval, John Guillebaud, Sunanda Gupta, Kate Guthrie, Susanna Hall, Philip C. Hannaford, Caroline Harvey, Mary Hernon, Lisa Iversen, Gabor Kovacs, Ali A. Kubba, Kathleen McNamee, Nicholas Panay, Tina Peers, Victoria Sephton, Sven O. Skouby, Lesley Smith, Anne Szarewski, Rik H. W. van Lunsen, Catherine White
- Edited by Paula Briggs, Gabor Kovacs, Monash University, Victoria
- Edited in consultation with John Guillebaud, University College London
-
- Book:
- Contraception
- Published online:
- 05 August 2013
- Print publication:
- 11 July 2013, pp vii-viii
-
- Chapter
- Export citation
Contributors
-
- By Blair C. Armstrong, David A. Balota, Lawrence W. Barsalou, Jos J. A. Van Berkum, Lera Boroditsky, Gregory A. Bryant, Cristina Cacciari, Joana Cholin, Morten H. Christiansen, Stella Christie, Eve V. Clark, Herbert H. Clark, Eliana Colunga, John F. Connolly, Michael J. Cortese, Seana Coulson, George S. Cree, Christopher M. Crew, Gary S. Dell, Kevin Diependaele, Judit Druks, Thomas A. Farmer, Anne Fernald, Kelly Forbes, Carol A. Fowler, Michael Frank, Stephen J. Frost, Dedre Gentner, Raymond W. Gibbs, Monica Gonzalez-Marquez, Arthur C. Graesser, Jonathan Grainger, Zenzi M. Griffin, Mary Hare, Harlan D. Harris, Marc F. Joanisse, Leonard Katz, Albert Kim, Gina R. Kuperberg, Nicole Landi, Birte Loenneker-Rodman, Danielle S. MacNamara, James S. Magnuson, Ken McRae, W. Einar Mencl, Daniel Mirman, Jennifer B. Misyak, Srini Narayanan, Kate Nation, Randy L. Newman, Lee Osterhout, Roberto Padovani, Karalyn Patterson, Kenneth R. Pugh, Terry Regier, Douglas Roland, Jay G. Rueckl, Vasile Rus, Jenny R. Saffran, Sarah D. Sahni, Arthur G. Samuel, Rebecca Sandak, Dominiek Sandra, Sophie Scott, Mark S. Seidenberg, Linda B. Smith, Michael J. Spivey, Meghan Sumner, Daniel Tranel, Gabriella Vigliocco, Nicole L. Wilson, Anna Woollams
- Edited by Michael Spivey, Ken McRae, University of Western Ontario, Marc Joanisse, University of Western Ontario
-
- Book:
- The Cambridge Handbook of Psycholinguistics
- Published online:
- 05 November 2012
- Print publication:
- 20 August 2012, pp xi-xiv
-
- Chapter
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Contributors
-
- By Osvaldo P. Almeida, Rebecca Anglin, Vivek Benegal, Margaret N. Berry, Nash N. Boutros, Henry Brodaty, Alan S. Brown, Monte S. Buchsbaum, William Burke, Kim Burns, Stanley V. Catts, Vibeke S. Catts, Jennifer M. Connolly, David L. Copolov, Louisa Degenhardt, Stewart L. Einfeld, Anthony Feinstein, Matt P. Galloway, Bangalore N. Gangadhar, Wayne Hall, Malcolm Hopwood, Michael D. Jibson, Ripu D. Jindal, David J. Kavanagh, Sophie Kavanagh, Matcheri S. Keshavan, Ennapadam S. Krishnamoorthy, Rajeev Kumar, Alexander F. Kurz, Nicola T. Lautenschlager, Edward C. Lauterbach, Leslie Lester-Burns, Lyn-May Lim, Jeffrey C. L. Looi, Michael Mazurek, Serge A. Mitelman, Ramon Mocellin, Bryan Mowry, Kim T. Mueser, Anand K. Pandurangi, Eric M. Pihlgren, Seethalakshmi Ramanathan, Patricia I. Rosebush, Perminder S. Sachdev, Richard D. Sanders, Vandana Shashi, Arabella Smith, Sergio E. Starkstein, Ezra S. Susser, Rajiv Tandon, Jagadisha Thirthalli, Bruce J. Tonge, Julian Trollor, Dennis Velakoulis, Mark Walterfang, Jane Zhang
- Edited by Perminder S. Sachdev, University of New South Wales, Sydney, Matcheri S. Keshavan
-
- Book:
- Secondary Schizophrenia
- Published online:
- 05 August 2011
- Print publication:
- 04 February 2010, pp vii-xii
-
- Chapter
- Export citation
Zoonotic infections in Northern Ireland farmers
- C. F. Stanford, J. H. Connolly, W. A. Ellis, E. T. M. Smyth, P. V. Coyle, W. I. Montgomery, D. I. H. Simpson
-
- Journal:
- Epidemiology & Infection / Volume 105 / Issue 3 / December 1990
- Published online by Cambridge University Press:
- 15 May 2009, pp. 565-570
-
- Article
-
- You have access Access
- Export citation
-
Evidence of past zoonotic infection was investigated serologically in randomly selected Northern Ireland farmers. The percentage of farmers with antibody was: Brucella abortus (0·7), Leptospira interrogans serovars (8·1), Borrelia burgdorferi (14·3), Toxoplasma gondii (73·5), Coxiella burnetii (28·0), Chlamydia psittaci (11·1) and Hantavirus (1·2).
The results show that Northern Ireland farmers have been exposed in the past to zoonotic infections. It is not known if these infections contributed to ill health in farmers but it is now time for the health of farm workers and their medical services to be reassessed.